faster, 30-45% more scans daily
radiologists in network
diagnostic cases in first 6 months
Context
Rad!olance was the first platform of its kind in the country. Before it existed, scans were burned to disks and sent by post because email wasn't compliant. Turnaround took days. Documents got lost. If you needed a specialist three cities away, you were stuck.
I owned the full design process: research, IA, MVP scope definition, role-based permissions, error states, and a design system built for a three-person clinical team.
Before the platform existed:
Physical delivery of medical data - scans were printed or burned to disks and sent by post due to security and legal constraints
Long diagnostic delays - clinics waited days for reports, regardless of scan complexity
Lost or damaged documents - no reliable way to track cases end to end
Uneven access to specialists - diagnostic quality depended on clinic location
No process visibility - clinics had no insight into case status or turnaround
High operational risk - compliance relied on manual handling and trust
After the platform launch:
Secure digital case workflows — imaging requests, reviews, and reports handled end to end
Faster diagnostic turnaround — radiologists could review cases remotely, independent of location
Full traceability and accountability — every case tracked from submission to delivery
Nationwide specialist access — clinics connected with radiologists across the country
Clear role-based workflows — admins, radiologists, and heads of radiology worked without friction
Reduced reliance on physical processes — postal delivery replaced by compliant digital infrastructure
The physical delivery process
12 days from scan to final result, with multiple delivery trips and waiting states. No tracking, no recovery if documents got lost.

Constraints
Why early decisions carried real risk
24 interviews across all three roles — 7 administrators, 12 radiologists, 5 heads — conducted within tight clinical and legal constraints. Early in discovery, I worked with legal and compliance teams to understand medical data regulations — these constraints shaped everything from file upload flows to role-based permissions. Security and compliance were non-negotiable. The key risk was moving forward with imperfect information, knowing that waiting would stall the project entirely.
Research
3 research schemes - pain points / impact mapping / existing workflow
Pain points by role, potential impact areas, and the day-to-day workflow before the platform existed.


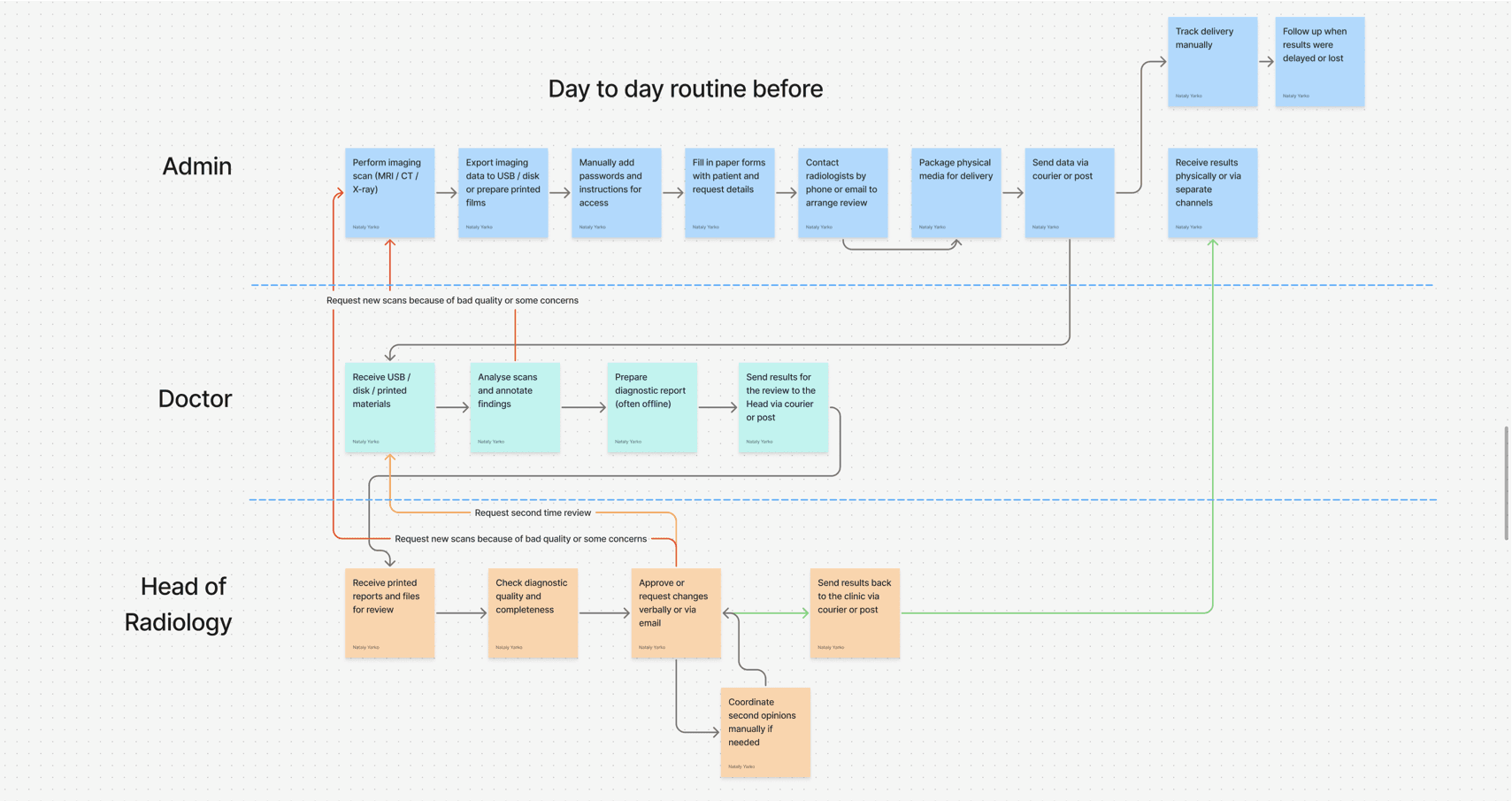
The key tension:
Conflict:
The problem was clear: physical delivery was killing them. Days of waiting, documents lost in transit, no way to track anything. But the research revealed something deeper: people weren't just afraid of the old system failing. They were afraid the new system would fail differently.
Digital uploads could fail silently. Cases could get stuck between roles with no visibility. A radiologist might accept a case that another radiologist had already taken. The risk wasn't building something slow — it was building something that looked fast but broke in ways they couldn't see or recover from.
My approach:
Moving forward with incomplete research felt risky in healthcare, but waiting would have killed the project. I tested rough concepts with all three user types at once to surface conflicts early. When research was thin, I made choices that favoured transparency and recoverability.
I partnered with the engineering lead to validate that the case-based architecture was technically feasible within our 3-month timeline. We prototyped the core workflow together before committing to the full design system.
Result:
The platform could earn trust from first use and evolve as real usage replaced assumptions.
Case workflow architecture
Cases move through the system with clear handoffs between roles. Notifications trigger at each step (10m-15m, 5m-15m timing shown in blue), decision points handle edge cases (need second opinion?), and every state is visible and recoverable. This architecture made failures visible instead of silent.

Insights
The decision that shaped everything
We considered structuring the platform around files — upload a scan, attach a report. It was simpler to build. But files don't have status, ownership, or handoff points. If a radiologist accepted a case and then went offline, there was no way to reassign it or see it was stuck. A case could hold state, move between roles, and recover. That single architectural decision made the platform trustworthy rather than just functional.
Design
From fragmented workflows to a shared clinical system
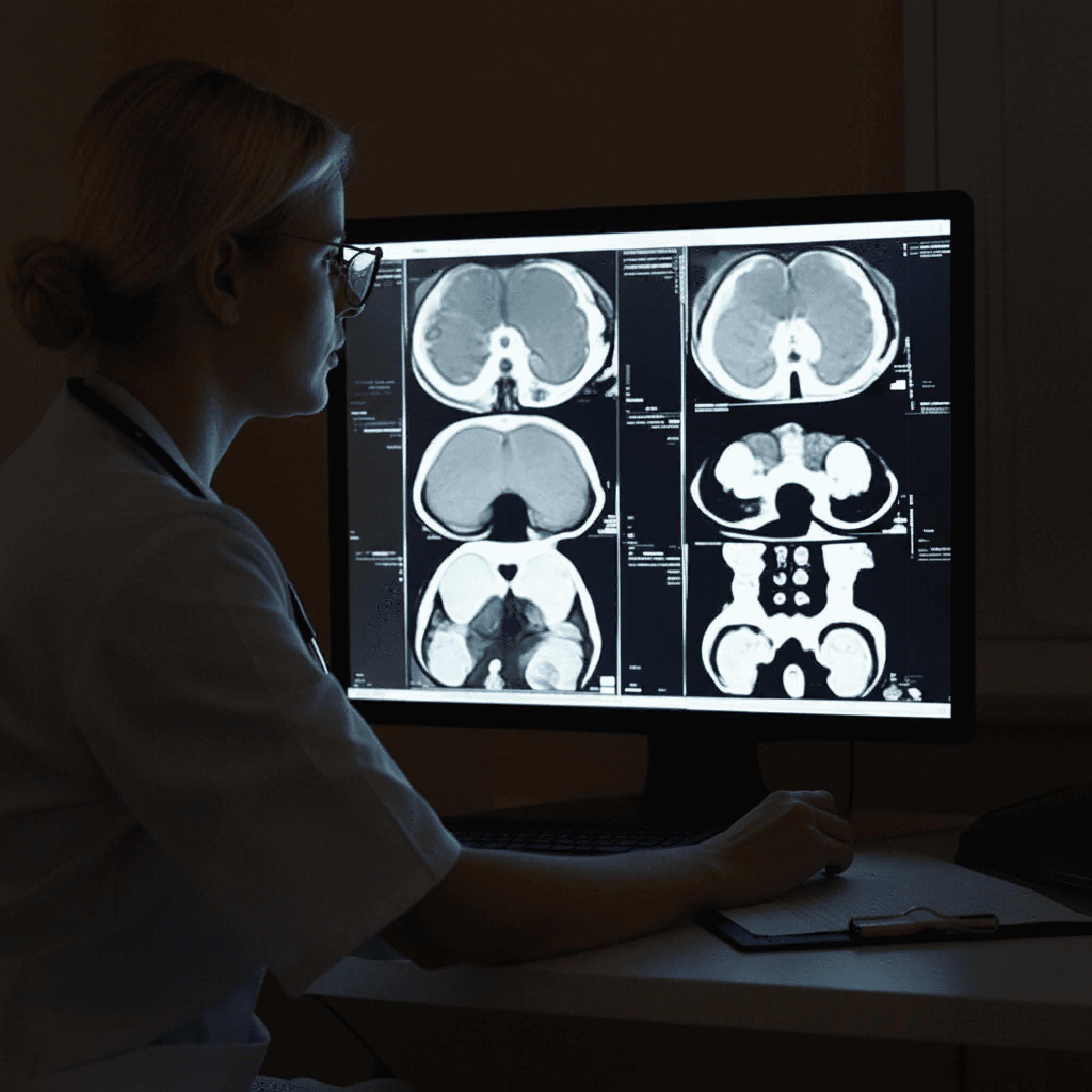
Reading room contrast.
Rad!ologists work in dark rooms. Admins work in bright offices. Each role needed completely different contrast and density.
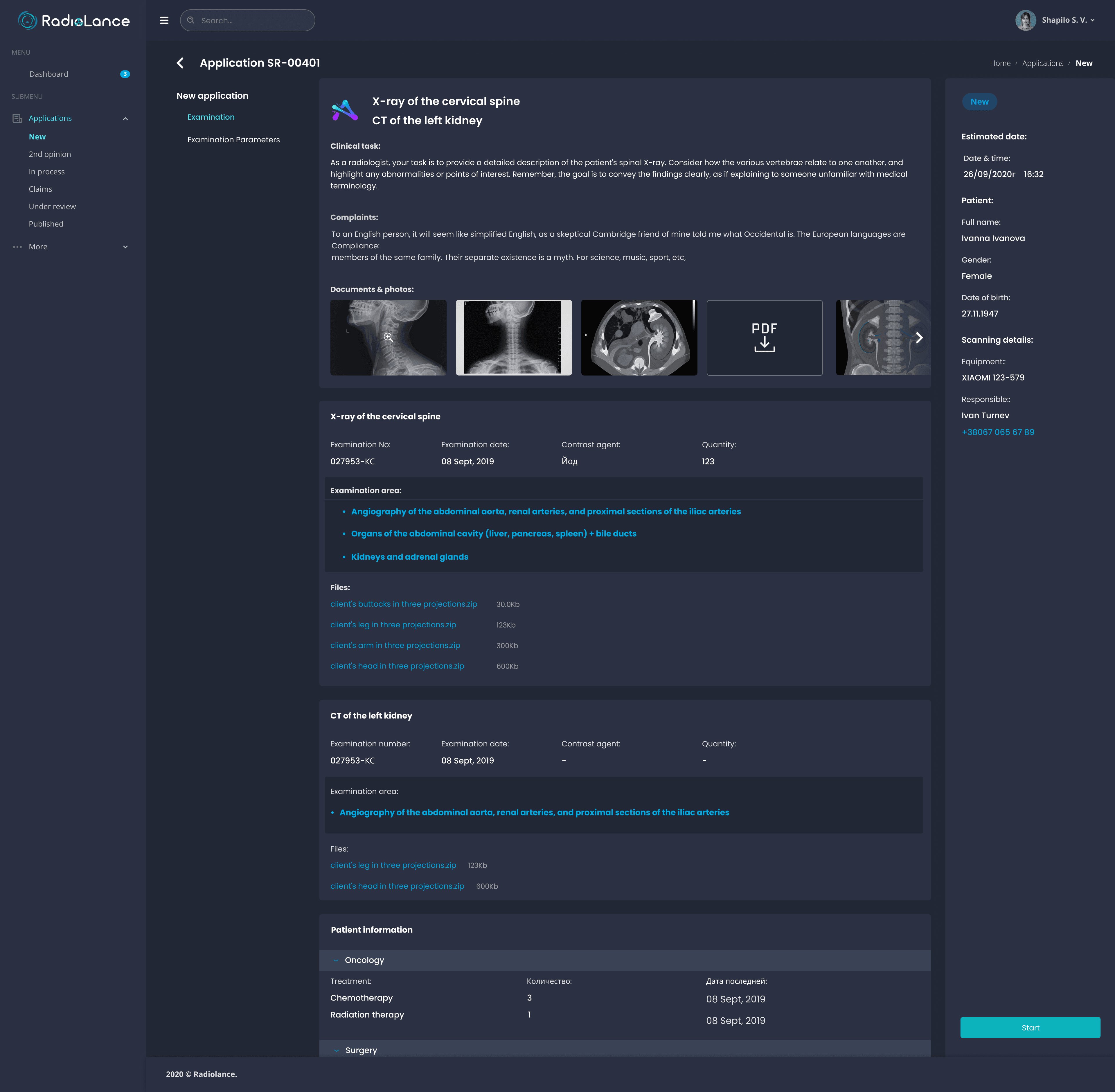
Case detail view with scan images
Case detail interface showing clinical information, patient data, and examination parameters alongside the actual medical scan. Dark UI optimized for reading rooms where radiologists spend hours reviewing imaging — every element designed for low-light environments without compromising scan visibility.
Streamlined approval.
Heads faced 50+ pending cases. One-click approval with clear hierarchy let them move quickly.
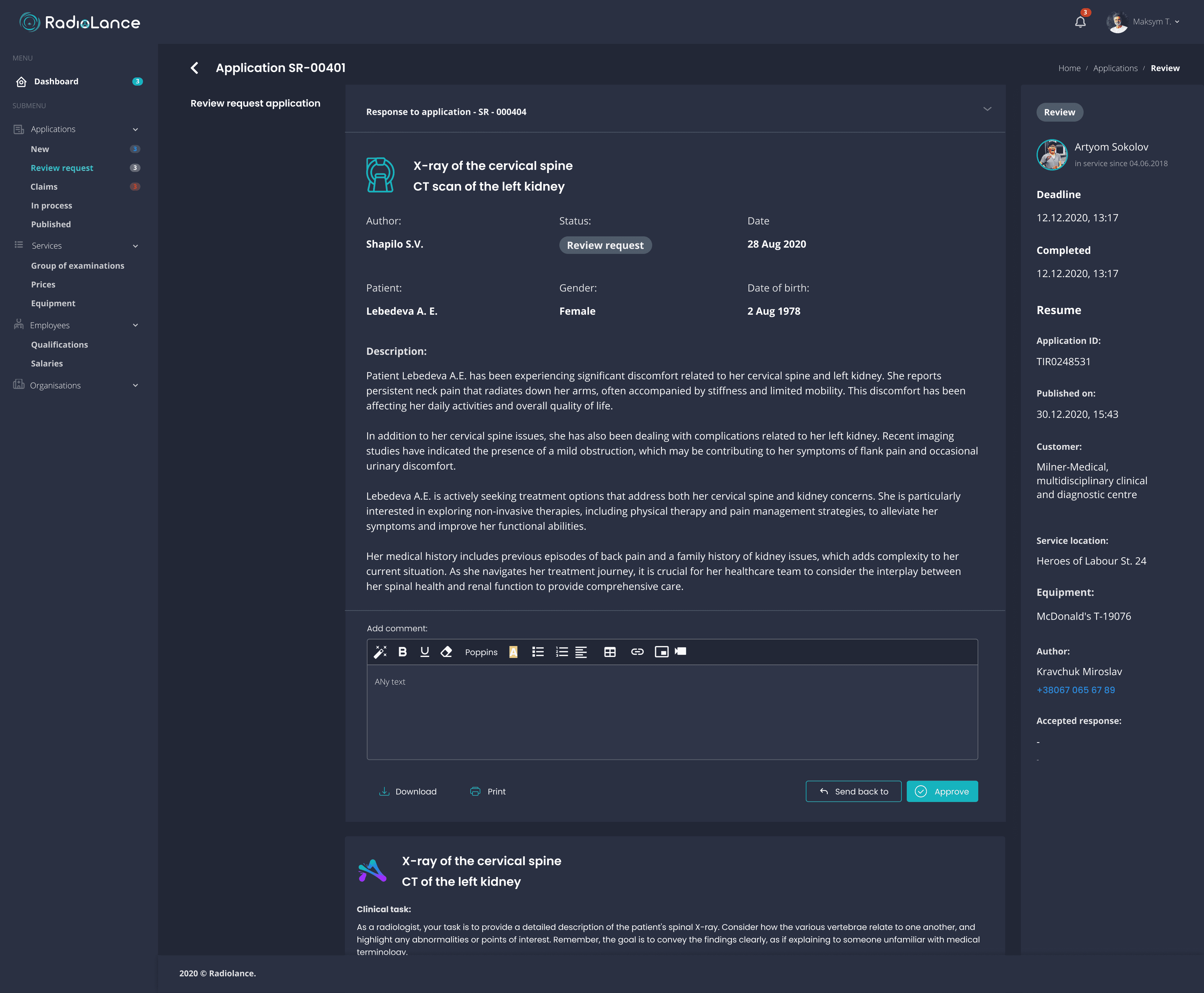
Management dashboard and approval workflow
Heads of radiology needed visibility across all cases (Applications, Clients, Contractors, Claims) with trend analysis to manage workload. The application detail view shows the complete case context with diagnostic description and one-click approval for final sign-off.

Upload reliability.
Before Rad!olance, clinics burned scans to CDs and printed physical images to send by post. The platform needed to make digital uploads faster and more reliable than the physical process they'd been using for years.
I worked with DevOps to design progress indicators and failure recovery that could handle large medical imaging files (15-20 minutes per upload). We tested upload flows with real clinic networks to ensure reliability under actual conditions.
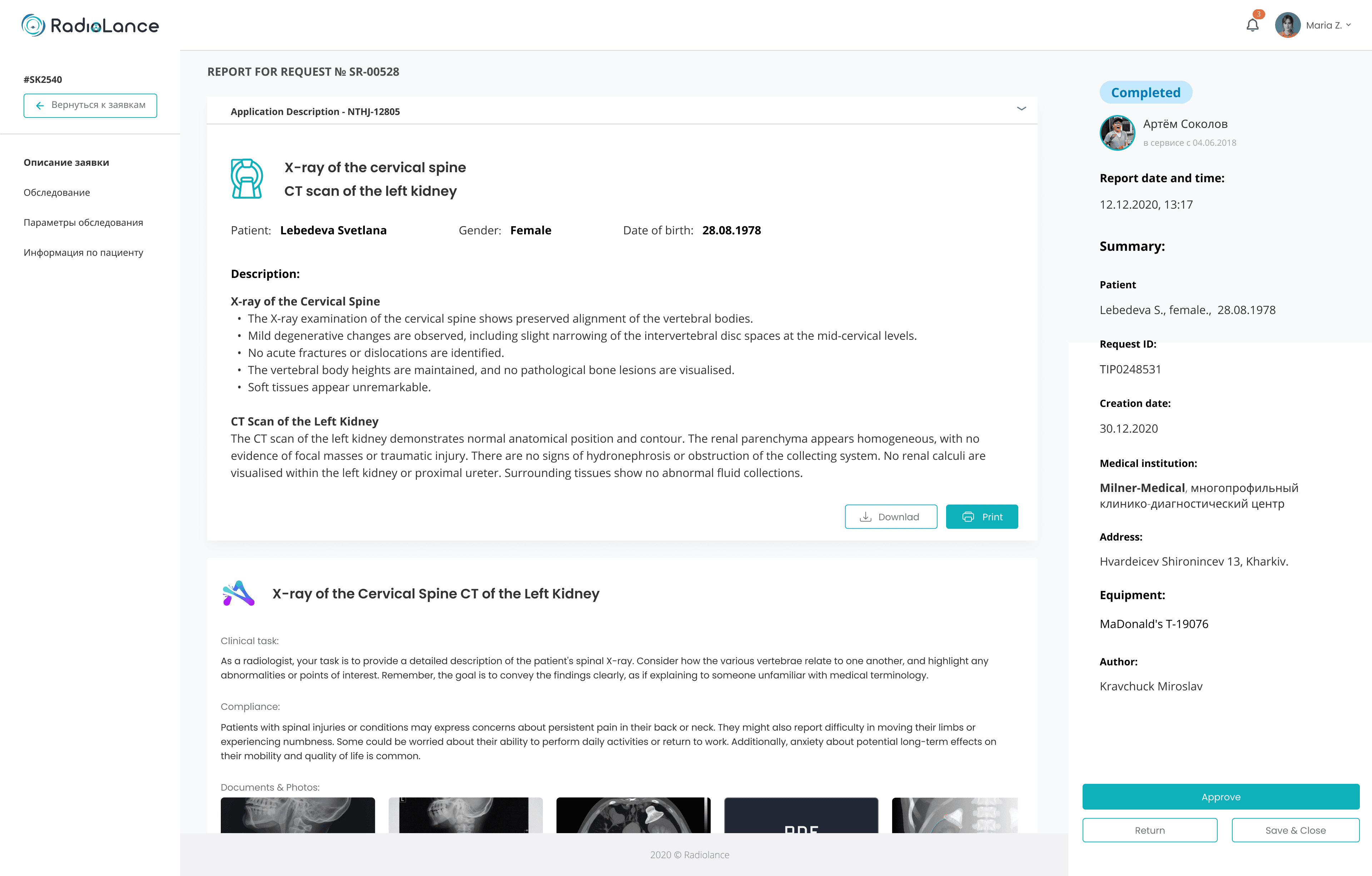
Admin interface and case tracking
Clinic admins work in bright offices, so they needed a light interface with clear application status tracking. The case detail view shows uploaded scan images and full diagnostic information — replacing the physical CD delivery process with instant digital access.

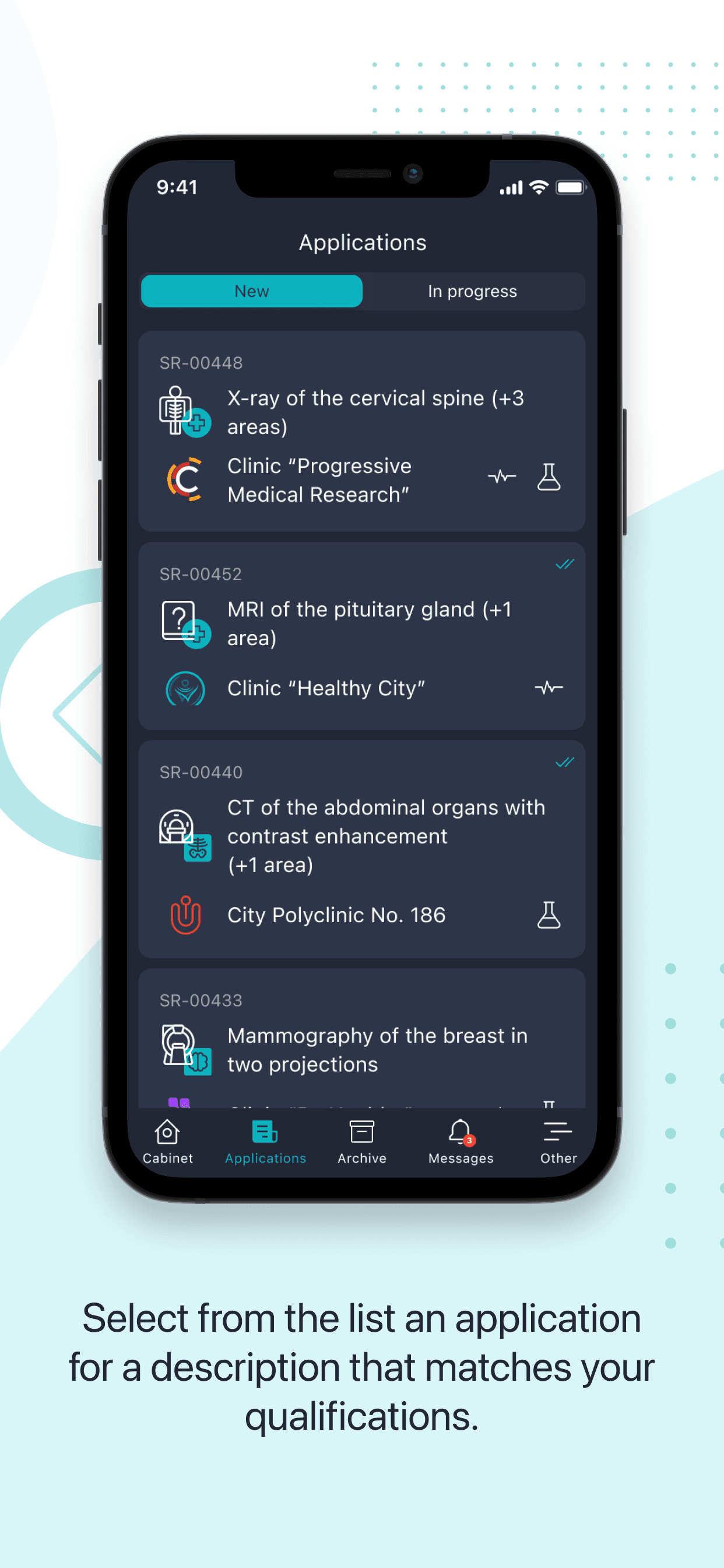
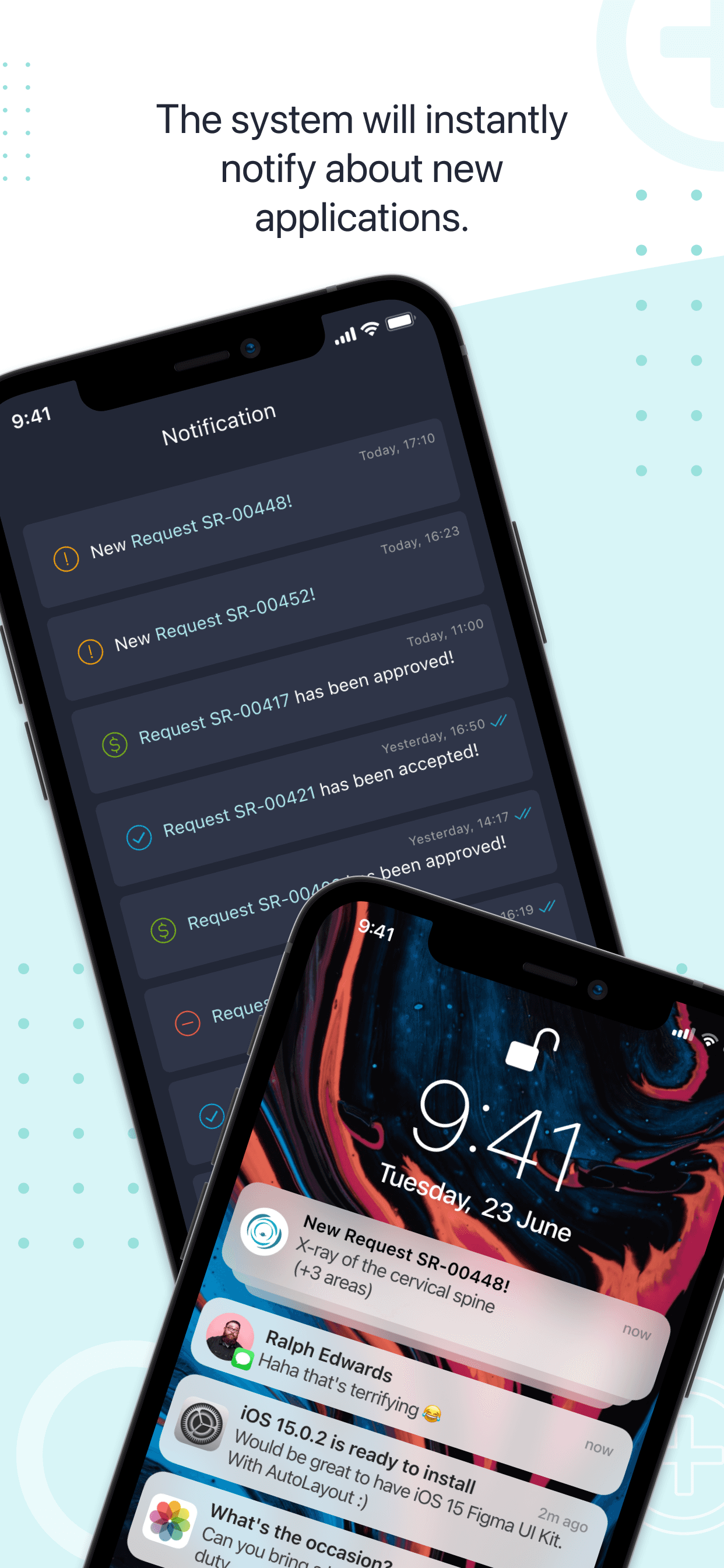
Mobile for radiologists.
I built the app so they could read case descriptions, accept or decline requests with one tap, and get push notifications. No more being chained to a desk.
Radiologists could browse available cases, see full clinical context (scan type, clinic, body areas, estimated time), and accept cases with one tap. Push notifications kept them updated on new requests and approvals without opening the app.


Validation
Did clinics actually switch from physical delivery?
The first signal was adoption speed. Within 6 months of launch, the platform had processed 1,500+ diagnostic cases — enough volume to confirm that clinics were replacing physical delivery, not just trialling the platform alongside it.
The bigger test was whether radiologists would trust a system they'd never used before. 70+ radiologists joined the network in that first period. They didn't have to — the old process still existed. That they chose the platform over familiar workarounds was the real validation.
The product is still live today, handling 150+ medical reports per day across public and private clinics nationwide. That's not launch momentum — that's a system that held.
Outcomes
From operational friction to scalable clinical infrastructure
3x faster processing from upload to approval. 30–45% more scans processed per day. Orders increased 30% as trust grew among both doctors and patients. Specialist access scaled nationally without increasing coordination overhead.
3x faster processing came primarily from the mobile accept/decline flow — radiologists could take cases from anywhere instead of being tied to a workstation
The product shifted the business from manual coordination to repeatable, scalable service delivery. It was the first platform to do so in the country.
"As the medical director of a private clinic, I appreciate the speed and predictability of working with Rad!oLance. Every day, we receive mammography and X-ray descriptions at the agreed time. If necessary, we request urgent descriptions within 2 hours. It is also very important for us that Rad!oLance operates officially based on a contract. A reliable and time-tested partner."
T. Bulanov,
Director of “Medibor” Clinic
"We have been working with Rad!oLance for over two years. They always take a thorough approach to describing and interpreting CT/mammography results. Deadlines have never been missed. During our collaboration, the number of orders has increased by 30%, which indicates trust from both doctors and patients."
A. Kovalyov,
Head of Valky Central District Hospital
Reflection
Trust is built in the failure states, not the happy path.
The biggest lesson was that in high-stakes systems, trust comes from what happens when things go wrong, not when they go right.
Building around cases instead of files, prioritizing recoverability over speed, making every handoff visible — these weren't UX decisions, they were trust decisions. Users didn't need the system to be fast on day one. They needed to know it wouldn't lose their work, wouldn't hide failures, and wouldn't make them guess what was happening.
In healthcare, every delay has a face. It's a patient waiting for a diagnosis that could change their treatment plan. It's a clinic that can't move forward until a specialist reviews the scan. It's a radiologist who needs to know whether the case they're looking at is the most urgent one, or if someone else already handled it.
That's why the foundation mattered more than any feature we could have shipped. A system that worked slowly but predictably was infinitely more valuable than one that promised speed but couldn't guarantee reliability. The first system people would use. The second they'd work around.
If I did it again, I'd push for a pilot with one clinic before full rollout. The client wanted to launch across all clinics at once, and we didn't push back hard enough. Some edge cases — like what happens when a radiologist accepts a case and the clinic uploads the wrong file format — only surfaced in production.
Error states - 404 and 500 pages with skeleton X-rays
Even error states were designed for the audience — 404 and 500 pages featured skeleton X-rays with dark humor that radiologists would appreciate.