Feature design
B2C | B2B SaaS
Digital Healthcare
Telemedicine

Physicians
working daily in the doctor dashboard
Patients
Appointments
per day through the scheduling flow
Context
Two healthcare platforms. Same system, completely isolated from each other. When COVID lockdowns started and doctors were seeing 150+ patients a day with no remote option, that gap stopped being inconvenient and became a crisis.
Two products, one system.
The situation I walked into
Medstar and Medcard24 both existed as separate MVPs. Medstar was the web platform for doctors and admins. Medcard24 was the patient-facing mobile app. Same healthcare system, completely isolated from each other.
Both had the same critical gaps: no online booking, no prescription requests, no doctor-patient messaging, no remote consultations, no way to track a patient's health between visits. In 2019 that was inconvenient. When lockdowns started and doctors were seeing 150+ patients a day in person, it became a crisis.
I was the sole designer across both products — user research, information architecture, prototyping, testing, and developer handoff. Medical data regulations shaped every flow from day one.
⚠️
Lockdowns made in-person care dangerous and unsustainable. Doctors were seeing over 150 patients a day with no remote alternative. Patients stayed home and went without care. The system needed a digital escape route, fast.
🔥
Doctor Burnout Risk
Unsustainable patient volume with no way to reduce in-person load
🚫
No Remote Option
The platform had no consultation flow outside physical visits
👴
Elderly Patients Stranded
High-risk patients couldn't safely access care
📋
Zero Scheduling Infrastructure
No digital way to manage or redistribute appointment load
Research
6 weeks. No time to wait for perfect answers.
We interviewed 5 doctors, 3 admins, and up to 10 patients — pulling in family members wherever we could. Alongside interviews, we ran unmoderated questionnaires so participants could answer in their own time while we used that window to design user flows in parallel.
Going in, we had no prior data. What we knew: GP clinics were collapsing under patient load with no remote option. That was enough to start.
Two things came out of research that weren't in the brief. The webcam gap — nearly half of patients didn't have one, which meant video-first would have excluded the people who needed remote care most. And elderly patients couldn't manage video or chat at all — we added a phone call request option specifically for them.
What we couldn't do: validate assumptions before building. Six weeks meant some decisions were made on instinct and corrected in testing.
Medstar — patient profile with some info

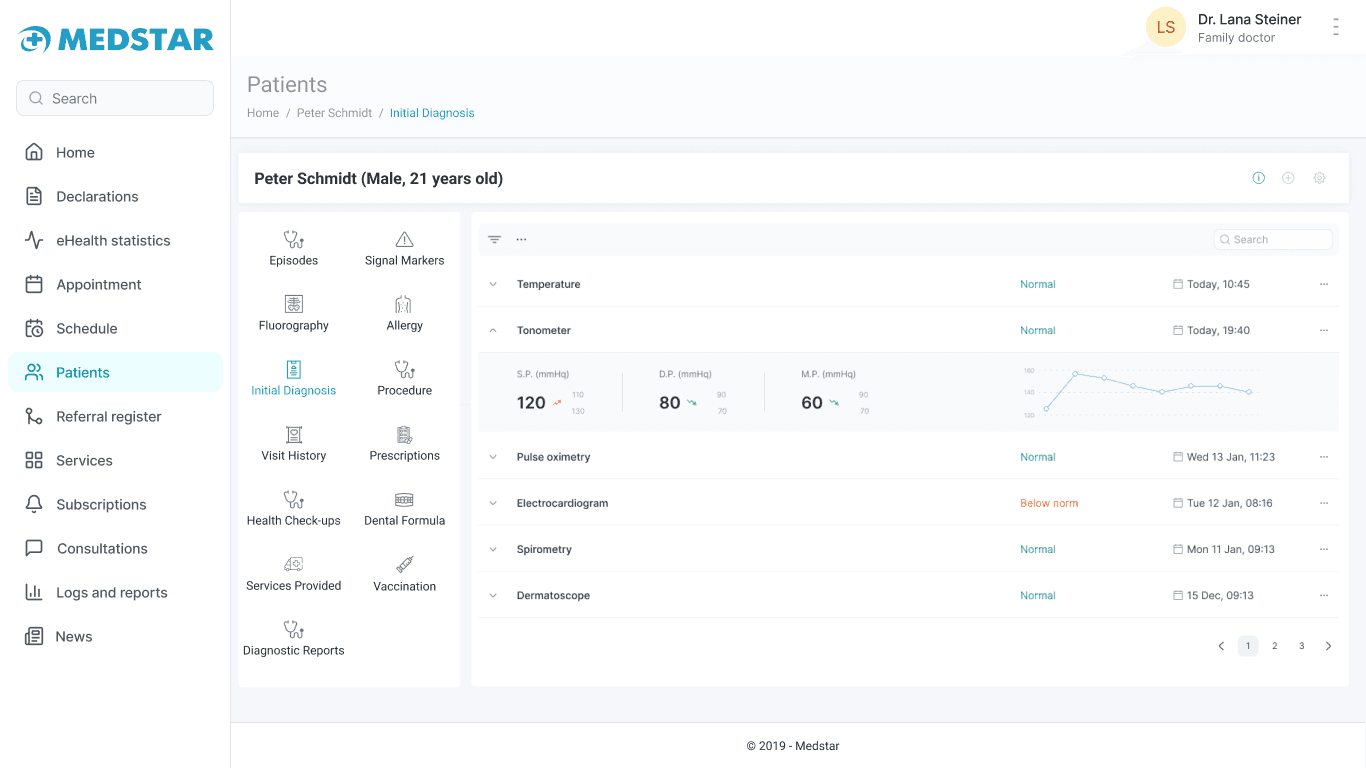
Insights
The problem we almost missed
We started with video calls as the primary consultation mode. Halfway through, testing with real patients revealed that nearly half of them didn't have a webcam — and most home computers simply don't come with one built in.
We'd been designing a video-first experience that would have excluded the people who needed it most.
Chat had to become a first-class experience — its own conversation structure, documented history, escalation paths — not a fallback. That decision clarified both products. In Medstar, doctors got a unified consultation view handling both modes. In Medcard24, patients were guided toward video or chat based on their device, neither feeling like the lesser option.
We also added an admin persona mid-project when it became clear doctors were still overwhelmed — because appointment distribution was still falling on them on top of everything else.
Medcard24 — patient vitals / wellness diary
Now patients can see and add their vitals
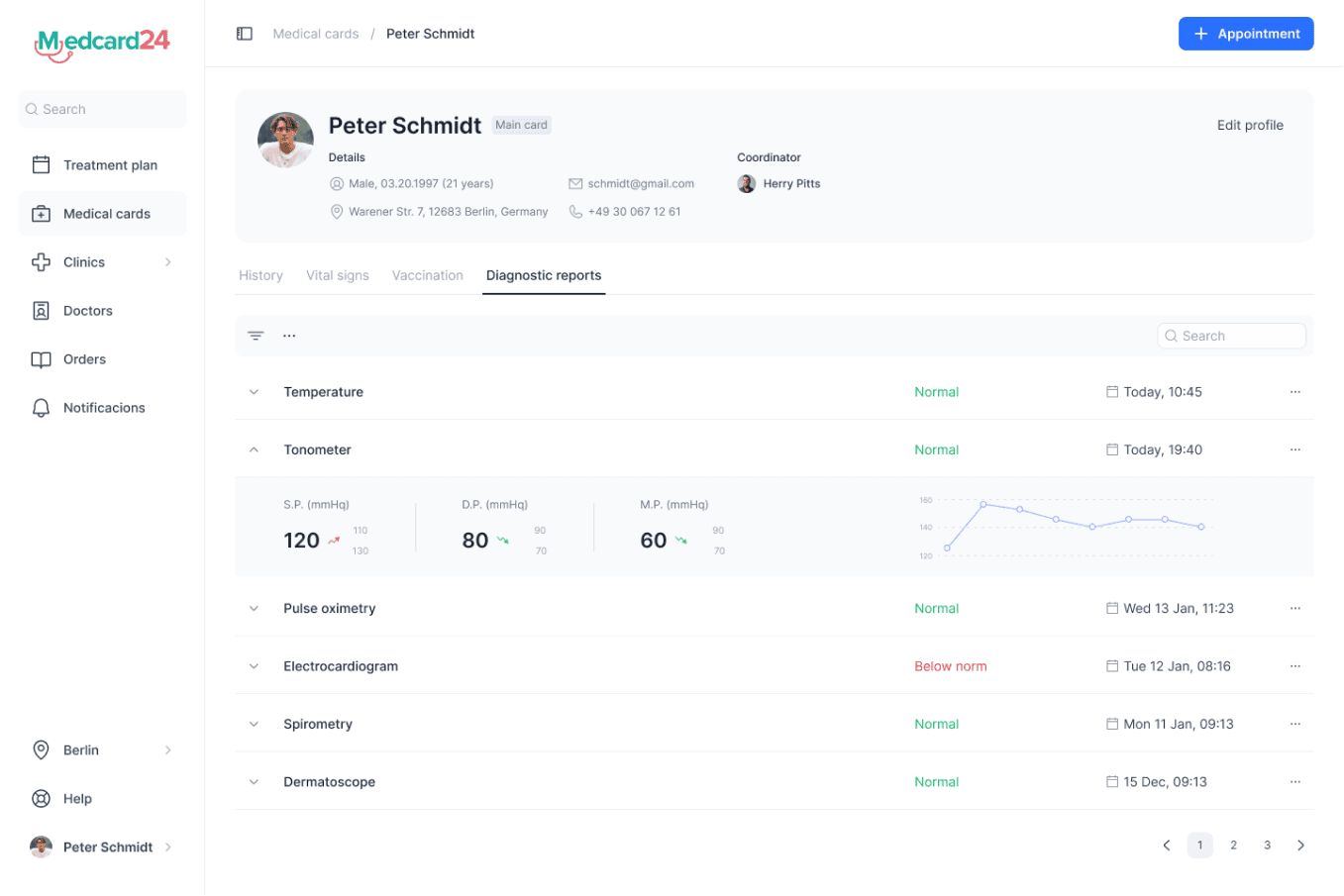
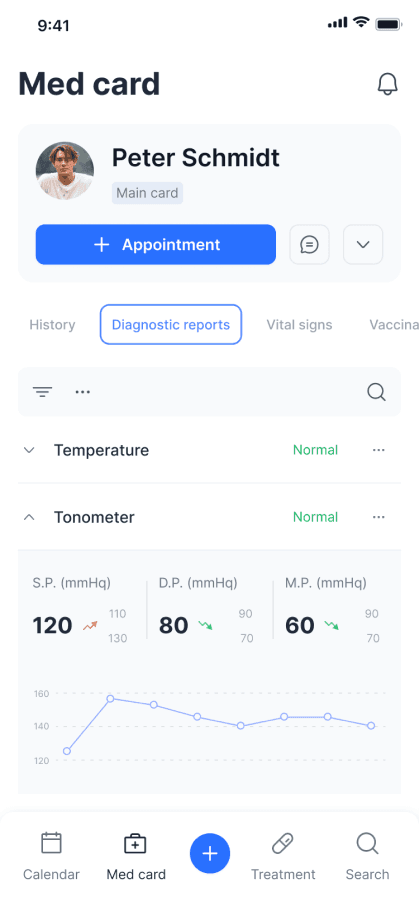
Ideation
What we built — and why
We didn't just add video calls. We asked what a remote consultation actually needs to be safe and complete.
That led to two features that weren't in the original brief. First, a wellness diary: patients log temperature, oxygen levels, and blood pressure daily inside Medcard24 — doctors see the full timeline in Medstar before and during a consultation. A remote call without clinical context isn't a consultation, it's a guess.
Second, medication delivery: we partnered with delivery services so patients could order prescriptions directly from the app. A digital prescription is useless if the patient still has to leave home to fill it.
Medstar & Medcard24— video consultation, waiting → live


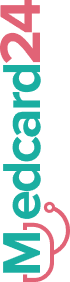

Validation
Did it hold under real lockdown conditions?
The 6-week launch happened during active lockdown — no controlled rollout, no soft launch. Doctors were already overwhelmed when the features went live.
The signal that it worked: offline patient visits dropped by half. Patients who couldn't leave home got consultations, prescriptions, and medication delivery without stepping outside. The system absorbed the load it was built for.
Longer term, Medcard24 reached 500K downloads on Google Play and a 4.8 App Store rating — in a market where people had no prior habit of managing healthcare on a phone. The platform now covers 15% of the Ukrainian healthcare market.
🏥
Before
🏥
Consultations
In-person visits only · Exposure risk for everyone during lockdown
📞
Appointment Booking
Call the clinic during working hours · Long queues, no visibility
📄
Patient records
Paper files · No digtal access for patients or remote doctors
👨⚕️
Doctor workload
150+ patients daily · No way to redistribute or reduce load
VS
📱
After
💻
Consultations
Video callor chat from home via Medcard24 app · No exposure
📅
Appointment Booking
Book online anytime · Admin manages schedule via Medstar dashboard
🗂️
Patient records
Full EHR in-app · History, prescriptions, and treatment plans in one place
⚖️
Doctor workload
Distributed across remote and in-person · Offline visits reduced by half
Outcomes
What changed
Offline patient visits dropped by half. Patients who couldn't leave home got consultations, prescriptions, and medication delivery without stepping outside. Doctors worked through lockdown with real clinical context.
Schedule — February 2021, full week view, colour-coded appointments. Admin persona managing load.

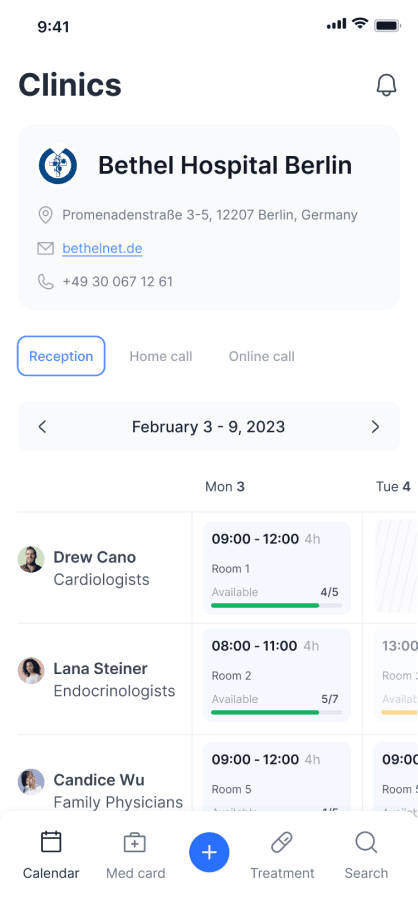
Clinics — Bethel Hospital Berlin, available booking slots. Patient-side booking infrastructure.

⚡
Core consultation flow designed and shipped during active lockdown
💬
Video + Chat
Two consultation modes so no patient gets excluded
👥
Multi-User Platform
Coordinated workflows for patients, doctors, and administrators
⚖️
Medical regulations shaped every flow from the start
♿
WCAG 2.1 compliant design for users across all age groups and abilities
🎯
Scheduling ownership removed from overloaded doctors
Reflection
What I learned
The wellness diary and medication delivery came from asking what the full experience needed to work — not what was on the brief. The webcam discovery came from testing with real users instead of assumed ones.
Both are the same lesson: the right question isn't "does the feature work?" It's "does it work for the person who actually needs it, in the situation they're actually in?"
In healthcare, that question isn't abstract. It changes every decision in the room.
We also added an admin persona mid-project when it became clear that appointment distribution was still falling on doctors. The solution wasn't always more features — sometimes it was redistributing work to the right person.


